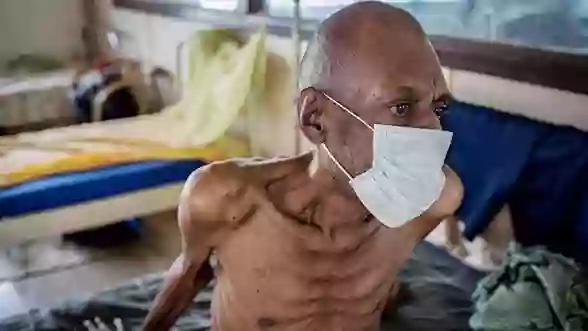
BY RITA OYIBOKA/AMAYINDI YAKUBU
The bus was already packed, bodies pressed into bodies, the stale mix of sweat and exhaust hanging thick in the air as it lurched through traffic. Then it started. A man near the window coughed with his mouth wide open. Once. Loud. Deep.
Heads turned.
He coughed again. This time, longer, rougher, the kind that seemed to claw its way out of his chest. A woman seated behind him shifted uncomfortably, pulling her scarf over her nose. By the third cough, she could not take it anymore. She stretched her head out of the window, desperate for clean air, but it was too late; the sound, the spray, the discomfort had already settled into the bus.
“Ah! You! Why don’t you cover your mouth when coughing? Haba, cover your mouth!” someone snapped from the back.
The man turned, irritated. “Should I not cough? Make cough kill me?”
Another voice cut in, sharper this time: “What if you have TB? You will give all of us TB!”
“God forbid! I don’t have TB! It is you who has TB! I be like person wen get TB?”
What followed was chaos, raised voices, accusations, and denial. But beneath the noise was something far more dangerous than the argument itself: ignorance, fear, and a disease that thrives in exactly that kind of environment, unnoticed, unchallenged, and spreading.
That disease is tuberculosis.
Marked every year on World Tuberculosis Day, March 24 is more than a date on the global health calendar. It commemorates the moment in 1882 when Robert Koch identified Mycobacterium tuberculosis, the bacterium responsible for TB, an achievement that laid the foundation for diagnosis and treatment. Yet, more than a century later, the disease remains stubbornly relevant.
Globally, tuberculosis continues to rank among the deadliest infectious diseases. In 2018 alone, 10 million people fell ill, and 1.5 million died. Today, the numbers remain alarming, about 4,100 deaths daily and nearly 27,000 new infections each day, despite the disease being both preventable and curable.
Nigeria sits at the epicentre of Africa’s tuberculosis crisis, and the numbers tell a story that is anything but linear. In 2020, the country recorded 138,591 cases, a figure that already raised concern among health experts. By 2023, however, the narrative appeared to shift; 371,019 TB cases were officially notified, surpassing national targets and accompanied by an impressive 93 per cent treatment success rate, suggesting that detection and response systems were gaining traction.
But that progress has not translated into a reduced burden. By 2025, Nigeria’s TB cases surged dramatically to 440,000, cementing its position as the highest TB-burdened country in Africa.
The numbers, taken together, reveal a dual reality: improved detection on one hand, and a stubborn, expanding epidemic on the other.
Under the 2026 theme, “Yes! We can end TB!”, the optimism is deliberate. But whether Nigeria can translate that optimism into reality remains a question hanging in the air, much like the disease is.
At a ministerial briefing in Abuja, the Coordinating Minister of Health and Social Welfare, Muhammad Ali Pate, made it clear that the country is pivoting. With dwindling global funding, Nigeria is now pushing toward domestic ownership of its health response, including a planned $346 million investment into TB, HIV, and malaria programmes in 2026.
The message is simple: dependence is no longer sustainable.
But policy declarations, as always, are the easy part. The real challenge lies in what happens on the ground, inside clinics, communities, and even overcrowded buses, where a single cough can ignite panic.
Ending TB Requires Execution Discipline, Not Just Funding – Umeh
Speaking with The Pointer, a medical doctor at the Federal Medical Centre, Asaba, Dr Charles Umeh argued that Nigeria’s biggest challenge is not ambition, but execution.
“The 2026 theme ‘Yes! We can end TB’, sounds optimistic. But let’s interrogate it. Can we really? Yes. Will we? That depends on whether we’re ready to fix structural inefficiencies. Nigeria’s biggest pivot right now is domestic financing, as highlighted by Muhammad Ali Pate. The planned $346 million injection into TB, HIV, and malaria programmes is a step in the right direction. But funding alone doesn’t solve execution gaps.
“TB control requires precision. Rapid testing, immediate treatment initiation, and strict adherence monitoring over six months or more. Break one link in that chain, and the system leaks. Now let’s talk transmission. Overcrowding is a multiplier. Think Lagos danfos, IDP camps in Borno, or one-room apartments housing five to eight people. TB thrives in these environments, not because people are poor per se, but because close, prolonged exposure increases risk.
“Another misconception I encounter constantly is how TB spreads. Many people don’t understand airborne transmission. They focus on contact, sweat, or blood, when in reality, prolonged inhalation of infected droplets in confined spaces is the primary risk. From a policy standpoint, awareness campaigns are still too generic. We need targeted, hyper-local communication, markets, motor parks, and religious centres. Not just billboards and radio jingles. If people don’t internalise the risk, they won’t act. And if they don’t act early, TB continues its quiet circulation.
“There’s also the issue of dependency. For years, Nigeria’s TB response has leaned heavily on donor funding, USAID, Global Fund, and NGOs. Now that global financing is tightening, we’re being forced to confront an uncomfortable truth that we built a system we don’t fully own. Ending TB will require decentralising testing to bring diagnostics closer to communities, digitising patient tracking to reduce loss to follow-up, incentivising adherence through transport support and nutrition, and making contact tracing aggressive and non-negotiable.
“Let’s not romanticise it. TB is curable, yes. But it’s also stubborn, social, and systemic. If Nigeria wants to hit the 2030 target, it has to move from policy announcements to ruthless execution discipline. Otherwise, we’ll still be having this same conversation, just with worse statistics.”
TB Blends In With Everyday Illness – Dr Igbinovia
Speaking with The Pointer, an Abuja-Based Infectious Disease Physician, Dr Osaze Igbinovia, explained that the real danger of tuberculosis lies not in its severity, but in its subtlety.
“Let me be blunt, TB is not dramatic at the beginning. That’s the problem. It doesn’t announce itself like people expect a ‘deadly disease’ to do. Take a typical case I saw last year concerning a commercial driver in Abuja. He came in after almost six weeks of a persistent cough. But he had already treated himself three times. First, malaria drugs. Then antibiotics from a chemist. Then herbal mixtures his uncle recommended. By the time he got to us, he had lost weight, developed night sweats, and was already infecting people around him.
“From his perspective, nothing was ‘serious’ at the start. Just fatigue, mild cough, maybe heat from the weather. Very relatable. Very common. That’s how TB wins: it blends in with everyday illness. Clinically, we know TB symptoms overlap with common respiratory infections. But what patients don’t realise is that TB operates on a slow-burning timeline. It can sit in the body quietly before it escalates. By the time symptoms become obvious, the patient has already passed through what we call the infectious window.
“Now layer stigma on top. Many patients suspect TB but delay testing because they don’t want the label. In some communities, TB is still quietly associated with HIV, poverty, or ‘unclean living.’ So people keep quiet, keep coughing, and keep spreading it. From a systems standpoint, the failure is not just medical, it’s behavioural. We’re dealing with a delayed health-seeking culture. Until that changes, early detection will remain a bottleneck, no matter how many free drugs the government provides.”
Why Nigeria’s Losing TB Fight At Grassroots – Nwamaka
Meanwhile, an Anatomist and First Aider in Ebonyi, Okogeri Nwamaka, noted that it remains difficult to detect and treat tuberculosis early in Nigeria, pointing to a mix of systemic and behavioural challenges.
“Sometimes, early detection is difficult due to a combination of health system gaps and patient-related factors such as low case detection, limited diagnostic capacity, poor access to healthcare, especially in rural areas, poor awareness, and stigma. Nigeria has one of the lowest TB detection rates globally, with a large number of cases not identified or reported.
“Some facilities lack modern diagnostic tools and equipment, and health workers may not be fully trained, especially for childhood TB detection, which is harder to diagnose. More so, rural, nomadic, and low-income populations have limited access to clinics and laboratories. Sometimes, distance and transport costs delay diagnosis.
“Again, many people don’t recognise symptoms early or delay seeking care due to ignorance, myths, or stigma. Some patients hide symptoms because TB is associated with shame. Also, weak health system factors like inconsistent drug supply, poor infrastructure, and limited coverage of TB services can equally affect treatment.”
Nwamaka further explained why structural conditions such as poverty and overcrowding continue to shape the spread and treatment of tuberculosis in Nigeria.
“Poverty and overcrowding are two of the strongest drivers of TB in Nigeria. They affect TB spread and treatment because TB mainly affects low-income populations, who are at high risk of infection, and due to poor nutrition resulting in weakened immunity, they can easily develop active TB.
“Again, poverty delays treatment. Even when treatment is free, patients struggle with transport to the hospital and proper feeding, because TB drugs require good nutrition. So many patients incur catastrophic costs despite free medical care.
“Overcrowding, on the other hand, increases transmission. TB spreads through the air, so crowded homes with poor ventilation allow rapid person-to-person spread. Poor living conditions worsen outcomes because malnutrition and overcrowding can lead to higher infection rates, treatment failure, and even death rates. Therefore, TB is not just a medical disease; it is strongly a social disease driven by poverty and overcrowding.”
She also outlined what must be done across all levels to curb the disease, stressing that responsibility must be shared.
“Government responsibilities should include increasing funding for TB programmes, expanding diagnostic services like more laboratories, GeneXpert machines, and rural outreach. The government should also integrate TB into all healthcare services, especially maternal, child health, and primary care, ensure consistent drug supply, and avoid stock-outs in treatment centres. In addition, they can provide transport, food support, and incentives for patients.
“Health workers’ role should include early suspicion and screening, testing any patient with a cough, and community outreach. There should be active case finding, not waiting for patients to come. They should educate patients, explain treatment duration and adherence, and reduce stigma by treating patients with confidentiality and respect.
“The public should learn to seek care early and not ignore a persistent cough. Patients should try to complete their treatment. Also, the public should avoid overcrowded and poorly ventilated spaces and support TB patients to reduce stigma.”
Nwamaka insisted that TB treatment is free across public health facilities, while noting that hidden costs still pose a challenge for many patients.
“TB treatment in Nigeria is free, but patients still face high indirect costs, which may affect adherence and outcomes. TB diagnosis in many public centres, anti-TB drugs, and drug-resistant TB treatment programmes are provided under the National TB and Leprosy Control Programme and are all free,” she said.
Ignorance, Stigma, Delay, That’s Where TB Hides – Samaila
At the grassroots level, where policies meet reality, Nurse Caleb Samaila of Family Health International 360 in Malfa, Borno State, sees the daily struggle up close.
“The issue we have here with TB is mostly in this country and the northern parts of Nigeria. TB has manifestations similar to those of many respiratory diseases. So, it looks familiar, but the infection doesn’t spread quickly. It depends on the individual’s body: the virus enters the body when it’s inhaled from the patient’s sputum. Some of the people it might take time before it manifests. Some of the people it manifests early. So, if it manifests early, it can be treated and cured.
“While other people can even take up to one to two months before the sudden symptoms of tuberculosis are noticed in the particular person’s body. So, some of the symptoms are that the person doesn’t like a very light place, and then night sweats when the person is shivering at night, sweated a lot. It is therefore very hard to treat it at an early stage because most people go through a draining period when they don’t experience specific symptoms in their bodies, and they don’t need to rush to the hospital. They might think it’s a normal fluid.”
Beyond symptoms, he challenges widely held assumptions about poverty and TB.
“Well, living conditions like poverty, first, poverty doesn’t actually affect tuberculosis because the government has made sure that all the treatments of tuberculosis are free. All of it is free, and it’s covered by USAID in hospitals, by NGOs, and by the federal government itself. So, it made it free.
“It’s only ignorance if you don’t have the knowledge or information about treating TB. So that’s the problem, because TB treatment is free. On the other hand, overcrowding, well, it affects people, and the spread of TB is quite very fast because TB can be transmitted through the sweat of that particular highly infectious person, through blood contact with that particular person.
“So, especially when that person spits, and it touches your body, and it links with your sweats, you’re definitely going to contract tuberculosis. When we come into contact with that person, especially during the incubation period, we say we are in the infectious stage. That stage is when a person is highly infectious, and any contact with them in an overcrowded environment means many people will contract it. A lot of people don’t really understand the treatment of tuberculosis because they fail to go to the hospital because of the stigma and also denial.”
For Caleb, the solution is straightforward but demanding: awareness, access, and action.
“The most prominent thing is creating awareness. The government should fund organisations to work within local communities. Community outreach is very important. If anyone is experiencing symptoms, they should come to the hospital immediately. The test and the treatment are free.”
Back on that bus, the argument fades, phones are lifted, and life resumes as usual. The man still coughs. The air remains shared. The danger, invisible and unacknowledged, lingers.
This is the reality of tuberculosis in Nigeria, not just in clinics, hospitals, or policy documents, but in everyday spaces: buses, homes, markets, and classrooms, where ignorance, stigma, and delay create fertile ground for the disease. The tools to fight TB exist. Treatments work. Funding is in motion, at least on paper. But the battle is bigger than medicine or money. It is a test of awareness, behaviour, trust, and execution.
Until Nigerians confront these harder truths, until communities act early, health systems function flawlessly, and stigma is stripped away, TB will continue doing what it does best: hiding in plain sight.
Ending it is not a question of possibility. The question is whether the country has the will to turn knowledge into action. And that, more than anything, is the fight still ahead. Because until that happens, TB will keep doing what it does best: hiding in plain sight.